Dr. Charul Bhanji
Technical Director
9821186618
© Copyright 2019. Regrow Biosciences Pvt Ltd. All Rights Reserved
FOR DOCTORS
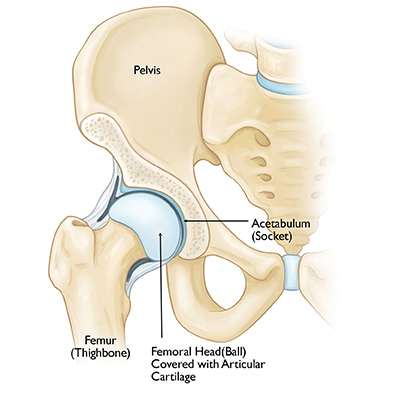
The hip joint is a ball and socket synovial joint, formed by an articulation between the pelvic acetabulum and the head of the femur. It forms a connection from the lower limb to the pelvic girdle, and thus is designed for stability and weight-bearing
AVN/ON is the localized death of bone tissue as a result of injury (trauma), drug side effects, or a pre-existing disease
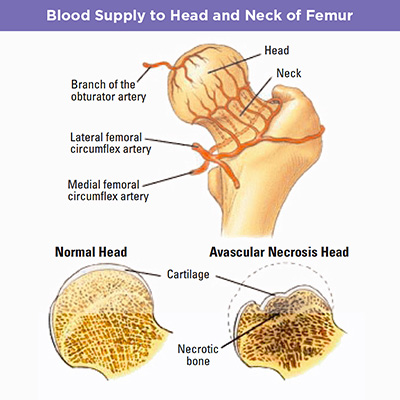
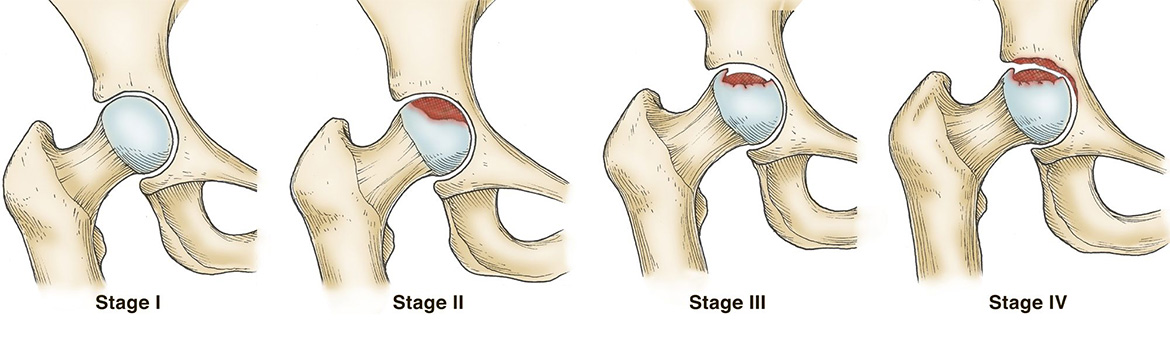
Progression of Disease
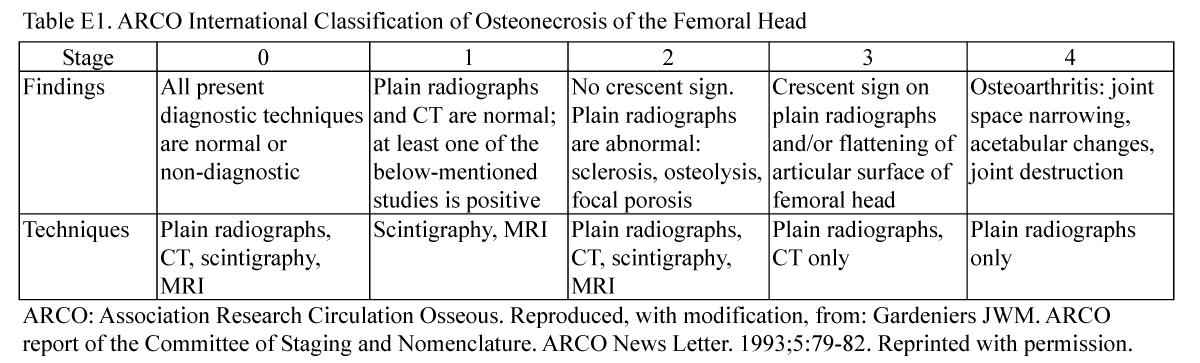
The Arco Classification Of Osteonecrosis
By the ARCO-Committee on Terminology and Staging
Classification:
Staging is a method of following the development of the disease and a way to start to treat the patient. Staging has to include the onset of the disease, Stage "0", and extend till the final end, the complete joint destruction.

How are we treating Avascular Necrosis Today?
Unmet Clinical need
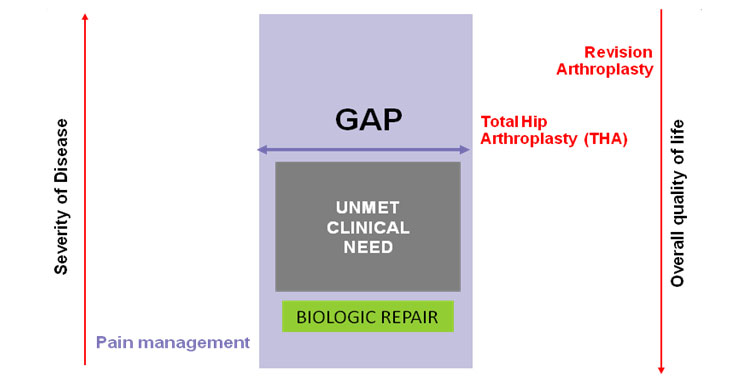
Biologic repair is now possible through Cell therapies such as Autologous Osteoblast Implantation
What is Autologous Adult Live Cultured Osteoblasts?
Goal of Treatment
Need for Globally approved treatments for Joint Preservation
Case Reports
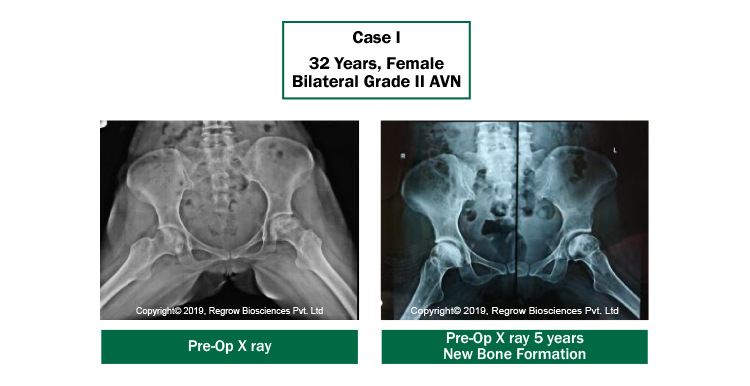
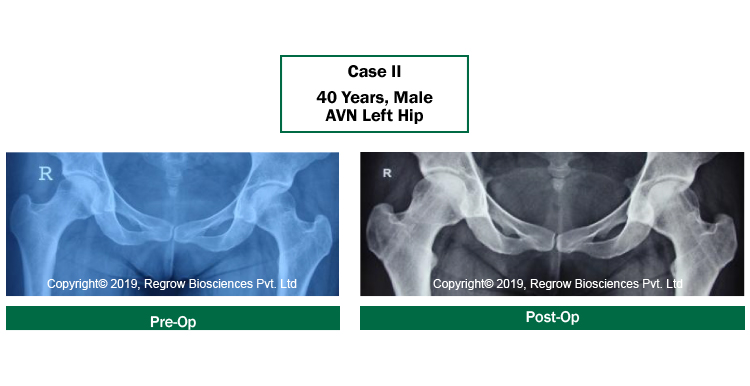
Our Process
Step 1
Bone Marrow Aspiration /Biopsy
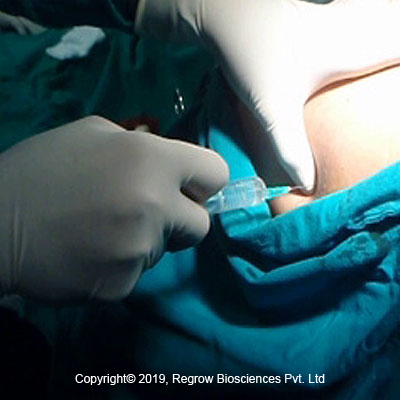
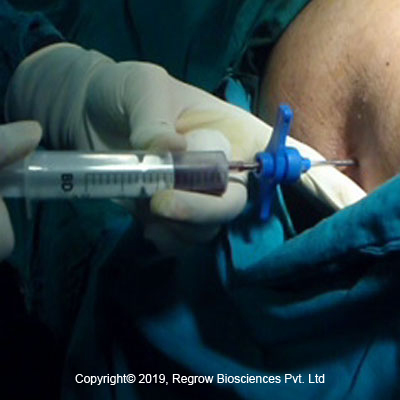
Step 2
Osteoblast Implantation
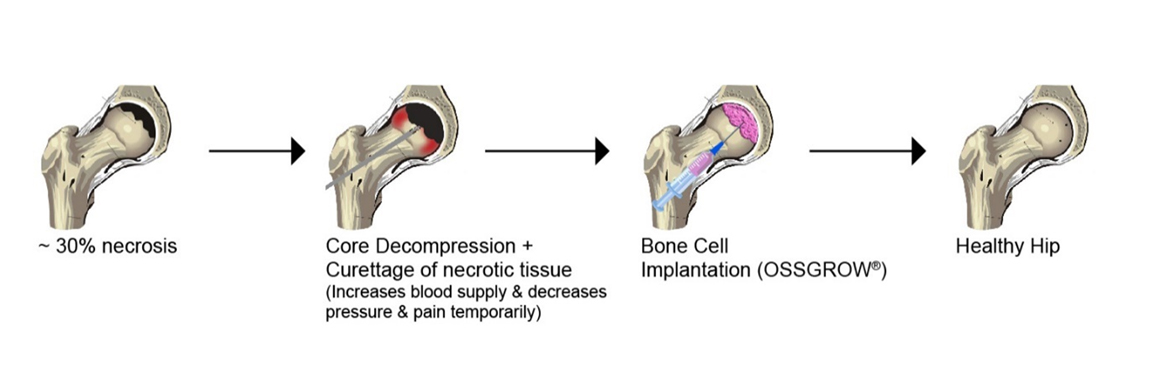
Implantation Procedure:
Billing and Insurance
To place the order or to know more about the product, please call :
Dr. Charul Bhanji
Technical Director
9821186618
Mr. Amos Chopade
Medical Officer
9619835838
Medical Education
Please refer to our academic library for peer reviewed International Publications on ACI
Coming Soon...
Coming Soon